RSNA Press Release
- Researchers studied the predictive value of whole-body MRI for the occurrence of major adverse cardiac and cerebrovascular events (MACCE) in diabetic patients.
- Patients who had detectable vascular changes on whole-body MRI faced a cumulative MACCE risk rate of 20 percent at three years and 35 percent at six years.
- Whole-body MRI may serve as a valuable noninvasive tool for assessing the risk of heart attacks and strokes in diabetic patients.
MRI May Predict Heart Attack and Stroke Risk in People with Diabetes
Released: September 10, 2013
| Media Contacts: | |
| RSNA Media Relations: | 1-630-590-7762 |
| Linda Brooks 1-630-590-7738 lbrooks@rsna.org |
Maureen Morley 1-630-590-7754 mmorley@rsna.org |
OAK BROOK, Ill. — Whole-body MRI may serve as a valuable noninvasive tool for assessing the risk of heart attack and stroke in diabetic patients, according to a new study published online in the journal Radiology.
Diabetes is a metabolic disease characterized by an increased concentration of glucose in the blood. There are 347 million diabetic patients worldwide, and the World Health Organization projects that diabetes will be the seventh leading cause of death by 2030.
Patients with diabetes are known to develop atherosclerosis, or thickening of the arterial walls, at an accelerated rate, resulting in a higher incidence of major adverse cardiac and cerebrovascular events (MACCE), such as a heart attack or stroke. However, there are wide variations in the degree of risk for adverse events among diabetic patients.
In recent years, whole-body MRI has emerged as a promising means to assess the cardiovascular systems of people with diabetes.
"One of the major advantages of whole-body MRI in this population is that the technique itself is not associated with radiation exposure, and larger body areas can be covered without increased risk, especially in younger patients," said Fabian Bamberg, M.D., M.P.H., from the Department of Radiology at Ludwig-Maximilians University in Munich, Germany. "As such, MRI can be used to evaluate the whole-body degree of disease burden that is not clinically apparent yet."
Dr. Bamberg and colleagues studied the predictive value of whole-body MRI for the occurrence of MACCE in 65 patients with diabetes. The patients underwent a contrast-enhanced whole-body MRI protocol, including brain, cardiac and vascular sequences. The researchers then conducted follow-up inquiries to assess the rate of MACCE in the study group.
Follow-up information was available for 61 patients. After a median of 5.8 years, 14 patients had experienced MACCE. Patients who had detectable vascular changes on whole-body MRI faced a cumulative MACCE risk rate of 20 percent at three years, and 35 percent at six years. None of the patients with a normal whole-body MRI went on to experience MACCE.
The findings point to a role for whole-body MRI as an accurate prognostic tool for diabetic patients that could speed effective treatments to those at risk, Dr. Bamberg said.
"Whole-body MRI may help in identifying patients who are at very high risk for future events and require intensified treatment or observation," he said. "Conversely, the absence of any changes on whole-body MRI may reassure diabetic patients that their risk for a heart attack, stroke or other major cardiac or cerebrovascular event is low."
Along with its prognostic accuracy, whole-body MRI has other advantages over existing methods of determining heart attack risk, according to Dr. Bamberg.
"Other established and valuable tools, such as myocardial perfusion imaging or computed tomography (CT) for quantification of coronary calcification, are generally limited to cardiac evaluation due to their associated risk profiles," he said. "Also, MRI provides unique insights into soft tissue pathology, including cerebral and vascular changes, such as restriction of blood flow to the brain."
Dr. Bamberg said that while whole-body MRI is a relatively recent development that needs more study, the results so far are promising.
"Our study provides preliminary evidence that the technique may be beneficial for risk stratification in patients with diabetes," he said. "We anticipate that emerging study findings in different diabetic cohorts will provide additional scientific basis to establish whole-body MRI as a screening modality."
# # #
"Diabetes Mellitus: Long-term Prognostic Value of Whole-Body MR Imaging for the Occurrence of Cardiac and Cerebrovascular Events." Collaborating with Dr. Bamberg were Klaus G. Parhofer, M.D., Elena Lochner, B.S., Roy P. Marcus, B.S., Daniel Theisen, M.D., Hannes M. Findeisen, M.D., Udo Hoffmann, M.D. M.P.H., Stefan O. Schönberg, M.D., Christopher L. Schlett, M.D., M.P.H., Maximilian F. Reiser, M.D., and Sabine Weckbach, M.D.
Radiology is edited by Herbert Y. Kressel, M.D., Harvard Medical School, Boston, Mass., and owned and published by the Radiological Society of North America, Inc. (http://radiology.rsna.org/)
RSNA is an association of more than 51,000 radiologists, radiation oncologists, medical physicists and related scientists, promoting excellence in patient care and health care delivery through education, research and technologic innovation. The Society is based in Oak Brook, Ill. (RSNA.org)
For patient-friendly information on MRI, visit RadiologyInfo.org.
Images
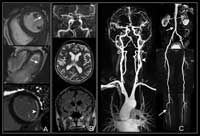 Figure 1. Whole-body MR images show multiple findings in 74-year-old man with type 2 diabetes for 21 years. A, Cardiac acquisi¬tions in short-axis (top image) and four-chamber (middle image) views show impaired function with anterolateral hypokinesia (arrows). Late gadolinium-enhanced image (bottom image) shows enhancement of anterolateral myocardium (arrowhead) indicative of MI. B, Cerebral acquisitions reveal normal cerebral arteries on time-of-flight angiogram (top image), axial T2-weighted brain image (middle image), and coronal fluid-attenuated inversion-recovery image (bottom image). C, Vascular acquisitions on contrast-enhanced MR angiograms demonstrate 50% stenosis of left internal carotid artery (arrowhead) and multisegmental luminal irregularities of abdo¬men (upper arrow), thighs, and lower leg with severe atherosclerotic disease and vessel occlusion (lower arrow). High-res (TIF) version (Right-click and Save As) |
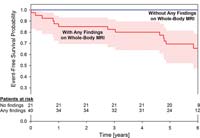 Figure 2. Kaplan-Meier survival curves for patients with and patients without any findings on whole-body MR images for occurrence of combined cerebrovascular and cardiovascular endpoint (MACCE) (P < .0001, log-rank test). High-res (TIF) version (Right-click and Save As) |
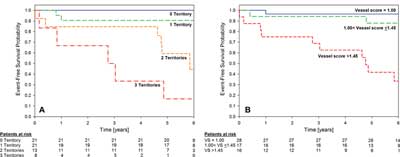 Figure 3. Kaplan-Meier survival curves for patients according to summary measures of whole-body MR imaging protocol for occurrence of combined cardiovas¬cular endpoint (MACCE). A, According to number of vascular territories with detectable changes on whole-body MR images (P .001, log-rank test), more vascular territories with detectable changes are associated with adverse outcome. B, According to tertiles of the MR imaging–based whole-body vessel score (VS) (P .0001, log-rank test), a higher vessel score is associated with adverse outcome. High-res (TIF) version (Right-click and Save As) |

 PDF
PDF